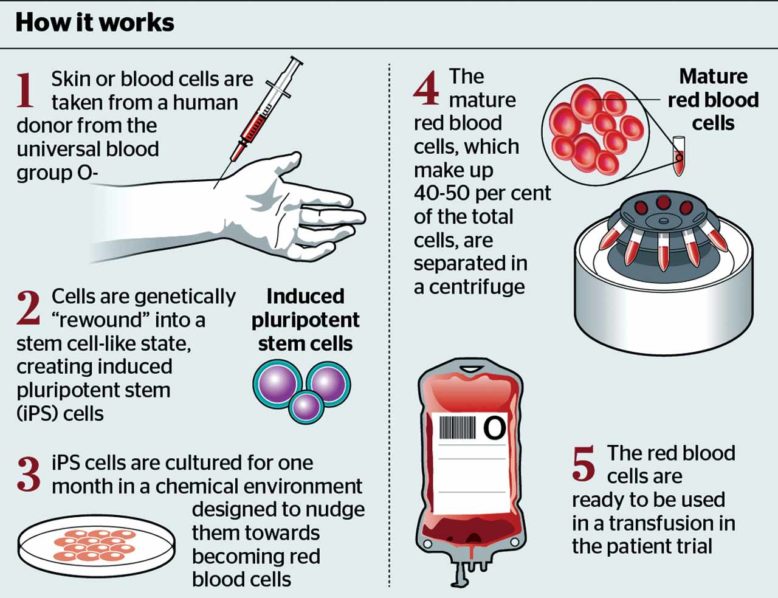
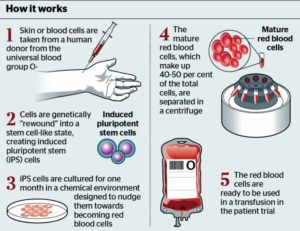
 Researchers have created an artificial red blood cell that effectively picks up oxygen in the lungs and delivers it to tissues throughout the body.
Researchers have created an artificial red blood cell that effectively picks up oxygen in the lungs and delivers it to tissues throughout the body.
Artificial blood stored as a powder could one day revolutionise emergency medicine and provide trauma victims a better chance of survival.
This artificial blood can be freeze-dried, making it easier for combat medics and paramedics to keep on hand for emergencies, said senior researcher Dr. Allan Doctor. He is a critical care specialist at Washington University School of Medicine in St. Louis, United States (U.S.).
“It’s a dried powder that looks like paprika, basically,” Doctor said. “It can be stored in an IV plastic bag that a medic would carry, either in their ambulance or in a backpack, for a year or more. When they need to use it, they spike the bag with sterile water, mix it, and it’s ready to inject right then and there.”
Also, a new study has found that an experimental drug may help reduce episodes of pain associated with sickle cell disease.
Results of an early trial showed the drug — called SelG1 for now — reduced episodes of sickle cell-related pain crises by 45 percent. In addition, the drug appeared safe and was well-tolerated, researchers say.
The study results were presented Sunday at the meeting of the American Society of Hematology, in San Diego. They were also published December 3 in the New England Journal of Medicine.
“Patients with sickle cell disease have complications, the most common of which is pain crises that require medical care and sometimes hospitalisation,” said lead researcher Dr. Kenneth Ataga. He’s director of the sickle cell programme at the University of North Carolina at Chapel Hill, United States.
Meanwhile, the artificial blood cell, which is about one-fiftieth the size of a normal red blood cell, is made from purified human haemoglobin proteins that have been coated with a synthetic polymer, Doctor said. Haemoglobin is the component inside red blood cells that carries oxygen throughout the body.
The hunt for an artificial blood substitute has been underway for more than 80 years, but the closest prior attempts have failed in two major ways, Doctor said.
Earlier versions could capture oxygen in the lungs, but then would not effectively release the oxygen after traveling out to tissues and organs, he said.
There also was an unintended reaction between “naked” haemoglobin and nitric oxide, a substance released by the lining of blood vessels that allows the vessels to relax and open up, Doctor noted.
“The haemoglobin consumes that molecule and causes a constriction of the blood vessels,” Doctor said. “When they tried to put naked haemoglobin into the bloodstream, it caused heart attacks and strokes.”
The synthetic polymer coating of the latest artificial blood cell appears to solve both these problems, Doctor explained. The coating was developed by the study’s lead researcher, Dipanjan Pan, an assistant professor of bioengineering with the University of Illinois at Urbana-Champaign.
The surface chemistry of the polymer reacts to the pH level of blood as it travels through the body, Doctor said. It captures oxygen when blood pH is high and releases oxygen when blood pH is low.
The polymer coating also keeps the haemoglobin from reacting with nitric oxide in the bloodstream, thus preventing dangerous constriction of the blood vessels, he added.
Lab tests involving mice and rats have proven that the artificial red blood cells can effectively deliver oxygen to needy tissues, the researchers reported.
Besides emergency settings, the artificial blood also could be used to help keep donated organs alive on route to a recipient, and supplement a hospital’s regular blood supplies during complex surgeries such as open-heart bypass, he suggested.
The artificial cell also is designed solely to deliver oxygen and leaves out a number of other functions that red blood cells provide.
Findings from the study are scheduled to be presented Saturday at the American Society of Hematology’s annual meeting, in San Diego. Study results presented at meetings are generally viewed as preliminary until they’ve been published in a peer-reviewed journal.